Here is how the COVID-19 pandemic is changing the way we view and experience grief
By Marin Wolf

Grief is hard to quantify.
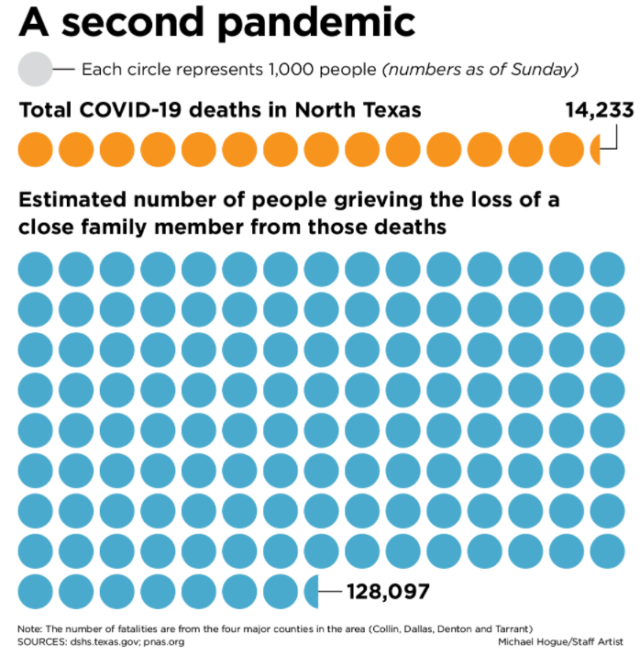
Yes, researchers can measure how long Texans have spent in the coronavirus pandemic (nearly two years); how many confirmed cases there have been in the state (more than 5.4 million); and how many Texans have died from the virus (more than 83,000), with more than 14,200 dead in the four major counties of North Texas.
They can measure days of lockdown, days of school missed and the average time each person will spend in quarantine because of exposure to the virus.
They can even measure how many hospital beds are open, how many nurses we have needed and how many health care workers will walk away from the profession because of COVID-related burnout.
What they can’t measure is the unfathomable amount of loss caused by the coronavirus.
After four surges of multiple variants of COVID-19, the pandemic appears to be ebbing. Mask mandates are now lifted for many of us and life is moving on. But for those left behind by the victims of COVID, any sense of normal – any semblance of pre-pandemic life – is still a long time away.
A second, silent pandemic known as grief has gripped many in Texas and beyond who have lost loved ones.
If we try to return to life as we knew it without confronting the trauma inflicted by such loss, we risk detrimental effects to our mental, emotional and physical health, experts warn.
While there are resources available for grieving families – mostly run through private organizations and nonprofits – some advocates say that the government isn’t doing enough as we head into this grief pandemic.
Getting financial and emotional help first requires recognizing grief’s toll. Unlike many other cultures, our American one often ignores, rather than embraces, the fact that death is a natural, though extremely difficult, part of all of our lives.
“There is no definitive answer to grief, because our love doesn’t have an end,” said Allison Gilbert, a journalist and author who writes about grief and resilience. “We need to remind ourselves that our friend or coworker is going to be experiencing this loss as long as they live.”
Talking about loss is the first step in acknowledging its weight.
The impact of coronavirus grief is far-reaching. In 2020, researchers came up with an indicator to measure that impact called the COVID-19 bereavement multiplier. For every COVID death in the U.S., nine surviving Americans will lose a grandparent, parent, sibling, spouse or child, according to the analysis.
By that estimate, there are more than 747,000 people who have lost a close relative in Texas to the virus.
Among them is Kornitki Sledge, of Dallas, who lost both her mother and grandmother in a matter of weeks, thrusting her into the role of emotional caretaker for her entire family. She’s put on a tough exterior for her relatives while internally she feels like “a boat at sea with no sail.”
There’s Jennifer Garcia, of Fort Worth, who can’t walk into certain restaurants anymore because it reminds her of the last time she was there with her late father, Alex Arango. It hurts her to think of the music, snacks and memories he and his family enjoyed together.
And every evening, Carmen Achee, of Fort Worth, catches herself glancing at the clock, expecting her daily call from her father-in-law who died in August. Her phone never rings.
Despite all of the heartbreak brought on by COVID-19, the grief pandemic has also proven the power of human resilience. The pandemic may, experts say, change the way communities think about and process death for the better.
“I’ve been remarkably inspired and humbled by the ways in which people have found ways to take care of not only their own well-being, but to also support others,” said Adam Brown, associate professor of psychology at The New School for Social Research in New York.
Celebrations of life, evolving
Grieving a death during COVID-19 looks different from grieving during any other time in recent history. COVID patients often die alone in the hospital because of isolation protocols, forcing family members to let go of how they envisioned saying goodbye to a loved one.
Final hugs and hand squeezes frequently turn to final kisses blown through the screens of a video call.
That distance often continues through the mourning process. Social distancing and shut-down orders delayed or halted memorial services and religious gatherings, forcing communities to change the ways they acknowledge and memorialize loss.
“Rituals provide that sense of calm, that sense of protection, that sense of being able to refer to something familiar in many cases, if these are cultural or religious traditions. And that helps us make sense of what makes no sense, which is trying to come to terms with a loss that is so profound,” Gilbert said.
There are, of course, creative workarounds families have used to collectively mourn, from virtual memorials and religious services to socially distanced funerals.
Most bereavement support options for families mourning the death of a loved one are organized through private organizations, like churches or grief-specific non-profits.
In the wake of COVID, the Federal Emergency Management Agency is providing funeral funding assistance to families who experienced a death from the virus after Jan. 20, 2020.
But some groups, like bereavement care organization Evermore, say the government should be doing more to support grieving families.
The Family Medical Leave Act, which provides some protections for employees who need time off work for their or their family member’s medical care, largely does not extend coverage to bereavement leave. That leaves little space for families to properly mourn or take care of after-death responsibilities, Evermore argues.
COVID deaths – specifically the physically traumatic and often violent end met by people with the virus – could serve as a wake-up call for how American culture views dying, said Holly Prigerson, co-director of the Center for Research on End-of-Life Care at Cornell University.
Death is an unavoidable fact of life, but it can be hard to accept, especially when it’s sudden or unexpected. Few people who get COVID think they’ll die from the illness, even though that’s not representative of reality. More than one out every 100 people in the U.S. who contract the virus will die from it, according to Johns Hopkins University of Medicine Coronavirus Resource Center data.
Families often push for life-saving measures for their loved ones, like intubation, even when chances of survival are slim.
“It doesn’t bode well for the patient’s comfort or chances of survival or benefiting from these heroic measures,” Prigerson said. “We’ve published data that show that family members of patients who die in the [intensive care unit] have higher risk of post-traumatic stress disorder six months later and higher rates of prolonged grief disorder.”
New interventions are coming
Prigerson and others in end-of-life care are developing interventions to prepare family members in the ICU for what they’re likely to experience so that they can make level-headed decisions. Education about the reality of dying and death can help surviving family members better cope with loss.
“There does need to be some education about what futile, burdensome care looks like,” she said. “I think no one wants to be the person to say that there’s no hope. Especially a physician. They don’t want to say they can’t do anything, but they know it’s not helpful to anybody. And it’s just kind of this sad, very tragic game.”
There is little comfort to be found when a loved one dies from COVID. Questions surrounding whether more could have been done or whether one decision led to someone catching the virus are likely never to be answered.
For some families, finding closure has been difficult. COVID protocols prevented them from saying goodbye. In October 2020, Alex Arango died in the hospital without his loved ones at his side.
“I think that one thing that still kills me is knowing that I didn’t get to say goodbye,” said his wife Anita. “That is just something that tears at me, that I didn’t get to tell him that it was OK. That I would be OK.”
There is some solace to be found in the sheer number of families dealing with the same questions and sorrow.
“There is community and there’s strength in numbers,” Gilbert said. “When you can come together and feel a part of a community that also understands your pain, there is a sense of belonging and a sense of connection that can make some people feel stronger.”
Staff researcher Naomi Kaskela contributed to this report.










